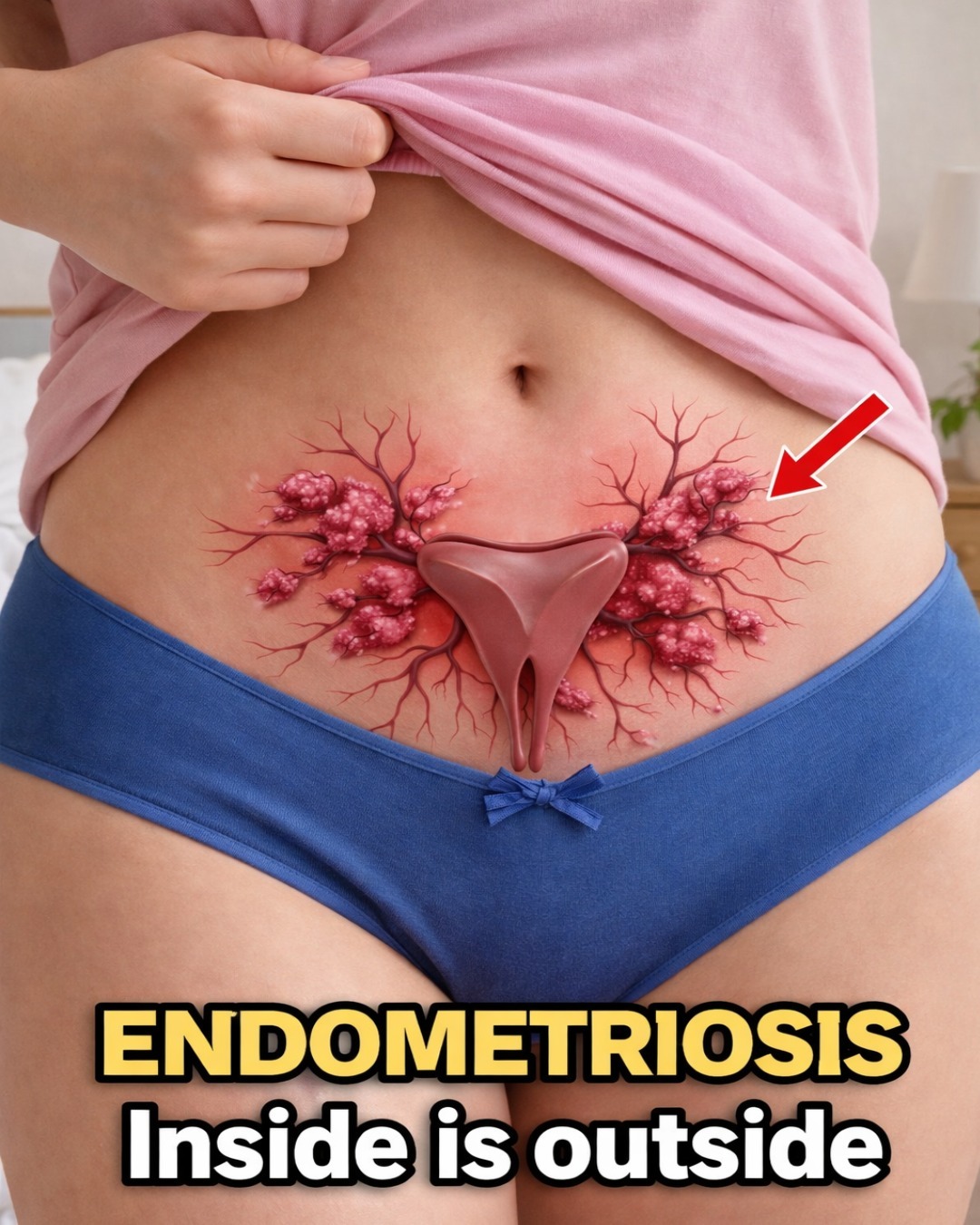
These stories aren’t rare. The average delay in diagnosis remains frustratingly long — often because women are taught to minimize their pain.
What Causes Endometriosis? The Current Understanding
Researchers don’t know the exact cause, but several factors appear to play a role:
Retrograde menstruation (menstrual blood flowing backward through the fallopian tubes)
Genetic predisposition — if your mother or sister has it, your risk rises
Immune system dysfunction
Hormonal influences, especially estrogen
Possible environmental factors
It’s likely a combination of these elements. Importantly, it’s not caused by anything you did or didn’t do.
Why Early Awareness Matters
Untreated or poorly managed endometriosis can lead to chronic inflammation, scar tissue, and reduced quality of life. Yet many women wait until the pain becomes unbearable.
Have you ever canceled plans because of period pain? Tracked your cycle obsessively trying to predict the worst days? Felt dismissed when describing your symptoms?
If yes, it’s time to listen to your body. Early conversation with a knowledgeable doctor can make a profound difference.
Diagnosis: What to Expect
There’s no simple blood test or scan that definitively diagnoses endometriosis (though ultrasound and MRI can help spot cysts or deep lesions). The gold standard remains laparoscopy — a minimally invasive surgery where a doctor views the pelvis and takes samples.
Don’t let that intimidate you. Many women say the confirmation brings enormous relief. Start by tracking symptoms in detail: pain levels, timing, and how they affect daily life. Bring this record to your appointment.
Treatment Options That Can Help
There is no cure yet, but symptoms can often be managed effectively. Options include:
Pain relief medications (NSAIDs)
Hormonal therapies (birth control pills, IUDs, GnRH agonists) to reduce estrogen and slow tissue growth
Surgery to remove lesions and adhesions
Lifestyle approaches: anti-inflammatory diet, regular gentle movement, stress management, and heat therapy
Many women combine approaches for the best results. What works varies by individual, so working with a specialist (often a gynecologist experienced in endometriosis) is key.
Lifestyle Strategies Many Women Find Helpful
While not a replacement for medical care, these steps support overall well-being:
Eat plenty of colorful vegetables, omega-3-rich foods (like salmon and walnuts), and reduce processed items
Move your body daily — walking, yoga, or swimming can ease stiffness and improve circulation
Prioritize sleep and stress reduction techniques
Track your cycle and symptoms with an app to spot patterns
When to See a Doctor
If pelvic pain disrupts your life, interferes with work, relationships, or sleep, or if you’re struggling to conceive, schedule an appointment. Bring a symptom diary. Be persistent — you know your body best.
You might be wondering, “What if it’s not endometriosis?” That’s okay. Getting answers rules things out and points you toward the right support.
Hope on the Horizon
Research continues into better diagnostics, non-hormonal treatments, and even potential preventive strategies. Awareness is growing, and more doctors are being trained to recognize the condition earlier.
You deserve to feel heard. You deserve answers. And you deserve tools that help you live fully, not just endure each month.
Continued on next page
For complete cooking times, go to the next page or click the Open button (>), and don't forget to SHARE with your Facebook friends.